Is My Cat Overweight? Cat Body Condition Score (BCS) AI Checker
Upload a side view and top-down photo of your cat — AI assesses body condition score (BCS 1–9), correctly identifies the primordial pouch vs true fat, and gives actionable diet guidance.
Photo 1 — Side View *
Drop your pet's photo here
or
✅JPG, PNG, WEBP
📏Max 8MB
This tool provides AI-generated preliminary analysis only. Not a substitute for professional veterinary diagnosis.
📸 Photo Guide
Good photos

Side view at body height

Top-down waist view
Avoid

Wrong angle — no waist info

Coat hides body shape
Tips for best results
- ✓Photo 1 (Side View): place your cat on a flat surface and photograph at their body height — crouch down to cat level for the correct angle
- ✓Photo 2 (Top-Down): stand directly above your cat and photograph straight down — both sides of the waist should be visible
- ✓Have your cat stand — sitting or curled positions hide the belly and waist shape entirely
- ✓Use natural daylight — indoor lighting can wash out body contours and make BCS harder to assess
- ✓The primordial pouch (loose belly flap) is NORMAL — our AI knows not to count it as fat
- ✓For long-coated cats (Persian, Maine Coon, Ragdoll): part the coat over the ribs, or photograph when coat is wet — AI will note when coat limits accuracy
- ✓For the side view, aim for the middle of the body — you should see the ribs, belly, and hindquarters in one frame
- ✓Compare to last month's photos — monthly BCS photos side by side catch slow weight gain that is otherwise invisible
How It Works — AI Cat Body Condition Score Checker

Step 1
Upload Two Photos
Take a side-view photo (cat at body height, belly and ribs visible) and a top-down photo (from directly above, waist shape visible). Two angles give the AI the best information for an accurate BCS assessment.

Step 2
AI Assesses Body Condition
Our AI identifies your cat's breed type, evaluates key visual markers — waist definition, rib visibility, abdominal tuck, hip prominence — and correctly distinguishes the normal primordial pouch from true excess fat.

Step 3
Get Your BCS Report
Receive a BCS score on the 1–9 scale with your cat's weight category (underweight / ideal / overweight / obese), plus specific diet recommendations. Long-haired breeds get a note on visual assessment limitations.
Cat Body Condition Score Guide — All 9 BCS Levels Explained
The 1–9 BCS scale is the veterinary standard for assessing body fat in cats. Scores 4–5 are ideal for most breeds. Here's what each category looks like and what to do — including the critical primordial pouch note. Also try our dog body condition score checker or cat skin checker or cat hair loss checker.
BCS 1–2: Severely Underweight
Emergency territory. Visible signs: ribs, spine, pelvis, and shoulder blades are ALL clearly visible from across the room with no touching required. No detectable fat; muscle wasting is visible, particularly over the hindquarters and spine. The cat may look angular or skeletal. Causes: advanced chronic illness (kidney disease, cancer, hyperthyroidism, IBD), prolonged starvation, severe dental disease preventing eating, or chronic malabsorption. In senior cats, unexpected severe weight loss is often the first sign of cancer or advanced organ disease. What to do: this is a veterinary emergency — do NOT wait. Vet visit within 24–48 hours. Never simply increase food without knowing why the cat is this underweight — feeding a cat with protein-losing kidney disease a high-protein diet can accelerate organ failure. CRITICAL WARNING: never fast a cat to "reset" appetite or for any reason. Even obese cats develop hepatic lipidosis (fatty liver disease) if they stop eating for 2–3 days. Any underweight cat that stops eating needs emergency vet care. Bloodwork, imaging, and sometimes a feeding tube are required.
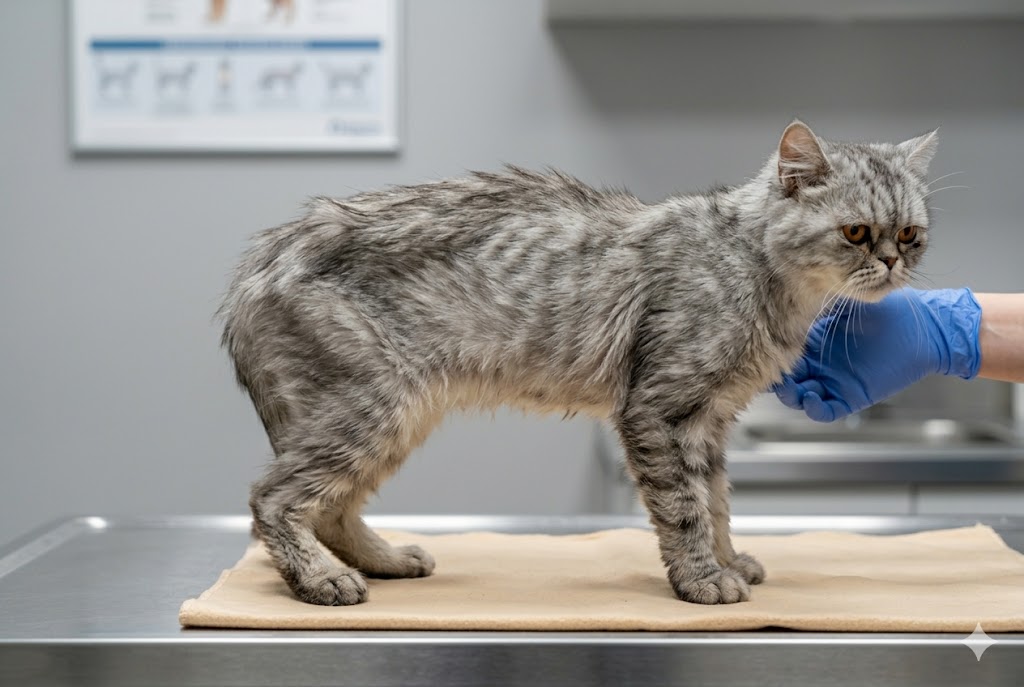
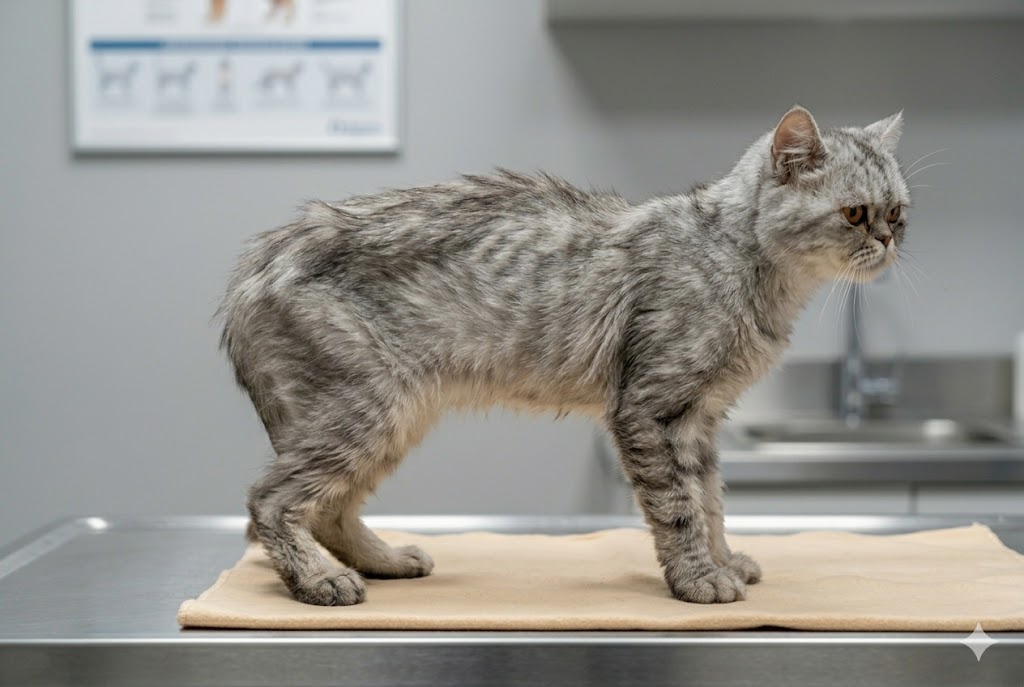
BCS 3: Underweight
Clearly underweight but not yet in emergency territory. Visible signs: ribs clearly visible without touching; pronounced bony points at hip and spine; very obvious hourglass shape from above with very little fill; abdominal tuck is extreme. Some muscle mass remains. Common causes in adult cats: dental pain (a leading cause in cats — tooth resorption and stomatitis are painful and common), hyperthyroidism (especially in cats over 10 — weight loss despite ravenous appetite is the hallmark sign), parasites (especially in young or outdoor cats), early kidney or inflammatory bowel disease. Recently adopted cats from rescues often present at BCS 3 — this is common and usually resolves. What to do: vet visit within a week. Key diagnostics: thyroid level check (T4) in any cat over 8 years; fecal parasite test; dental exam if the cat is eating slowly or dropping food. For otherwise healthy underweight cats: increase meal frequency to 3–4 smaller meals per day using a high-quality, high-protein wet food; avoid high-carbohydrate dry kibble (less nutritious per calorie); add a rotational protein (cooked chicken, fish) to increase palatability. Recheck BCS in 4 weeks. Goal: gain 0.5–1% body weight per week. NEVER use appetite-stimulating drugs without vet guidance in a cat that hasn't had a thyroid check.
BCS 4–5: Ideal Weight
The healthy target for most cats. BCS 5 is textbook ideal; BCS 4 (slightly lean) is also healthy and common in very active, young, or naturally lean breeds (Abyssinian, Siamese, Oriental Shorthair). Visual signs at BCS 5: ribs easily felt with gentle pressure but not visible; clear waist from above (inward curve behind the ribcage); slight abdominal tuck from the side; pelvis and spine palpable but not prominent. IMPORTANT: all cats have a PRIMORDIAL POUCH — a normal loose flap of skin and fat along the lower belly. Even at ideal BCS 4–5, this pouch may be quite visible, especially in older cats and certain breeds (Egyptian Mau, Savannah, Bengal, domestic shorthair). This is NOT fat — the primordial pouch does not affect BCS. The rib test overrides visual belly assessment. Health benefits of ideal BCS: reduced risk of feline diabetes (every BCS point over 5 significantly increases diabetes risk), lower joint stress, better anesthetic safety, and longer average lifespan. If your cat is at BCS 4–5: maintain current diet and exercise; do the rib test monthly; avoid free-choice feeding (most cats overeat when food is always available).


BCS 6: Slightly Overweight
The earliest overweight stage — and the easiest to correct. Visual signs: ribs palpable but require more than light pressure; waist is visible from above but less defined than ideal; abdominal tuck is reduced or absent; there may be a small fat pad at the belly beyond the normal primordial pouch. BCS 6 is very common post-spay/neuter (metabolic rate drops 20–30%), in indoor cats without active play, and as cats transition from young adult to middle-aged (4–7 years). Many owners don't recognize BCS 6 because the cat still looks "normal" — but this is the time to act. What to do: no vet visit required if otherwise healthy. (1) Weigh all food with a kitchen scale — measuring cups underestimate by up to 30%. (2) Reduce daily food by 10%. (3) Add two 10–15 minute interactive play sessions daily (wand toy, laser). (4) Cut treats to ≤5% of daily calories or eliminate entirely. (5) Switch to wet/canned food if currently on dry-only — wet food has fewer calories per gram and provides hydration. (6) Recheck BCS in 4 weeks. Goal: return to BCS 5 within 2–3 months. Target loss: no more than 1–2% body weight per week. Never cut more than 20% of calories at once — hepatic lipidosis risk.
BCS 7: Overweight
Clinically overweight — carries real health consequences in cats. Visual signs: ribs difficult to feel even with firm pressure (buried under fat); no visible waist from above — body is a rounded tube; belly may be pendulous beyond the primordial pouch; fat deposits over hips and at base of tail. Estimates suggest 35–50% of pet cats in Western countries are overweight or obese. HEALTH RISKS specific to cats at BCS 7+: (1) DIABETES: obese cats have a 3–5× higher risk of developing feline type 2 diabetes — fat tissue causes insulin resistance. Some diabetic cats can go into remission with weight loss. (2) HEPATIC LIPIDOSIS RISK: any illness that reduces appetite in an obese cat can trigger rapid-onset fatty liver disease. (3) JOINT DISEASE: arthritis is common and often silent in cats (they mask pain). (4) URINARY: obese male cats have higher risk of urethral obstruction. (5) GROOMING: cats who cannot reach their lower back or base of tail due to belly girth develop matting and skin disease. What to do: vet visit within a week for baseline bloodwork (thyroid, blood glucose, kidney and liver panels). Weight loss plan: 10–15% caloric reduction from CURRENT intake; high-protein wet food (aim for 200–250 kcal/day for typical overweight cat); structured play twice daily; recheck BCS every 4 weeks. Target: 1–2% body weight per week maximum.

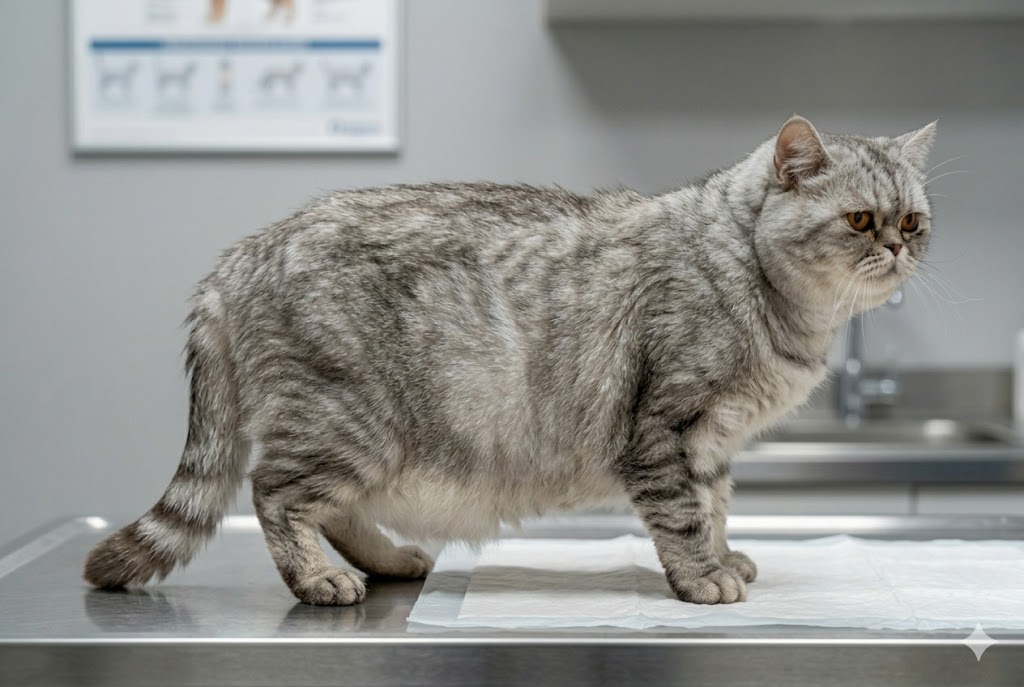
BCS 8–9: Obese
Obesity — requires veterinary intervention. Visual signs at BCS 8–9: ribs not palpable under thick fat layer; no waist from any angle; massive belly hangs down (well beyond normal primordial pouch); fat deposits form rolls over the neck, shoulders, and base of tail; waddling gait; extreme exercise intolerance (may refuse to play at all); difficulty grooming — the lower back, base of tail, and perineal area may be soiled. At BCS 9, cats may have fat-fold dermatitis (skin infections in deep fat rolls), breathing difficulty when resting, and may vocalize when moved or handled due to joint pain. MEDICAL EMERGENCIES to watch for in obese cats: (1) Hepatic lipidosis — if the cat stops eating for ANY reason, this is now an emergency because fat mobilization into the liver happens rapidly. (2) Diabetic ketoacidosis — if the cat is lethargic, vomiting, and not eating, suspect this. (3) Respiratory distress — fat around the chest wall restricts breathing especially when the cat lies on its side. What to do: veterinary consultation required. Do NOT attempt aggressive caloric restriction at home — the hepatic lipidosis risk is REAL. Prescription weight management diets (Hill's Metabolic, Royal Canin Satiety for Cats) are formulated to achieve weight loss while maintaining nutrition. Monthly vet weigh-ins and BCS checks are required. All household members must be aligned — one person sneaking extra food undermines the entire program.
Is your cat overweight, or is it just the primordial pouch?
Upload a side view and top-down photo — AI gives your cat a body condition score (BCS 1–9), correctly identifies the primordial pouch vs true fat, and provides specific diet guidance. Takes 30 seconds.
Check Cat Body Condition →Medical Disclaimer
PawCheck provides AI-generated preliminary health analysis for informational and educational purposes only. This service is not intended to replace professional veterinary advice, diagnosis, or treatment. The AI analysis has inherent limitations and may not always be accurate. Always seek the advice of a qualified, licensed veterinarian with any questions regarding your pet's health. Never disregard professional veterinary advice or delay in seeking it because of information provided by this tool. If your pet is experiencing a medical emergency, contact your veterinarian or emergency animal hospital immediately. By using this service, you acknowledge and agree to these terms.
Frequently Asked Questions
What is a good body condition score for a cat?
+
A body condition score (BCS) of 4 or 5 out of 9 is ideal for most cats. At BCS 5, you can feel the ribs easily with light pressure but cannot see them; there is a clear waist tuck behind the ribcage when viewed from above, and a slight abdominal tuck from the side. The average healthy adult cat weighs 3.5–5.5 kg (8–12 lbs) — but weight alone is unreliable because body size varies by breed. Maine Coons and Ragdolls are naturally large (6–8 kg), while Siamese cats are naturally lean. BCS accounts for body type rather than arbitrary weight targets. Think of the scale in thirds: BCS 1–3 = underweight, BCS 4–5 = ideal, BCS 6–7 = overweight, BCS 8–9 = obese. One important note: all cats have a PRIMORDIAL POUCH — a loose flap of skin and fat along the lower belly. This is normal anatomy and should NOT be mistaken for obesity. Upload a side + top-down photo for an AI assessment of your cat's BCS.
Is my cat fat or is it a primordial pouch?
+
This is the most common confusion in cat body condition assessment — and an important distinction. THE PRIMORDIAL POUCH is a loose flap of skin, fat, and connective tissue that hangs from the lower belly of all domestic cats. It swings from side to side when your cat walks or runs. It is completely NORMAL anatomy — not a sign of obesity — and serves as protection for the belly during fights and allows expansion when a cat eats a large meal. Even very lean cats (BCS 3–4) have a primordial pouch. FAT vs PRIMORDIAL POUCH: (1) The pouch hangs BELOW the belly line and moves with the cat; excess body fat is distributed everywhere — over the ribs, back, and base of the tail, not just the belly. (2) To check for true obesity, use the RIB TEST: run your fingers along the ribcage. In an ideal-weight cat, ribs are easily felt with light pressure. If you cannot feel the ribs despite firm pressure, your cat is likely overweight regardless of the pouch. (3) A WAIST CHECK from above: look down at your cat — you should see an inward curve (waist) behind the ribs. No waist = likely overweight; visible waist = healthy even with a noticeable pouch. Our AI specifically notes the primordial pouch distinction in its assessment.
How do I tell if my cat is overweight?
+
Three reliable at-home checks: (1) RIB TEST — place your hands on either side of your cat's ribcage and run your fingers gently along the ribs. In a healthy cat, individual ribs should be easy to feel with light pressure, like touching your knuckles. If you must press hard, or can't feel the ribs at all, your cat is likely overweight. (2) WAIST CHECK from above — look down at your cat from above. You should see a clear inward curve (waist) behind the ribcage. If the body is a straight-sided tube or rounded rectangle with no waist, that indicates overweight. (3) BELLY PROFILE from side — the belly should not hang down lower than the sternum (breastbone) when the cat stands. A pendulous belly BEYOND the primordial pouch — meaning the entire underside is rounded and sagging — signals excess fat. Other signs: reluctance to jump to their usual spots, tiring during play within seconds, difficulty grooming the base of the tail or lower back, waddling gait. Note: male cats and neutered cats are at higher risk of obesity — spaying/neutering reduces metabolic rate by up to 30%.
Is 12 pounds too heavy for a cat?
+
12 lbs (5.4 kg) is on the heavy side for most cats — but context matters enormously. For a small-framed female domestic cat, 12 lbs may represent BCS 7 (overweight). For a large-framed male cat or a large breed, 12 lbs may be completely normal. Reference ranges: (1) Average female cat: ideal 3.5–4.5 kg (8–10 lbs). Overweight threshold typically 5+ kg (11+ lbs). (2) Average male cat: ideal 4–5.5 kg (9–12 lbs). Overweight threshold typically 6+ kg (13+ lbs). (3) Maine Coon male: ideal 6–8 kg (13–18 lbs) — 12 lbs may actually be UNDERWEIGHT for this breed. (4) Siamese: naturally lean, ideal around 3.5–5 kg (8–11 lbs) — 12 lbs is overweight. The right question is not "how much does my cat weigh" but "can I feel the ribs easily, and is there a visible waist from above?" A cat at 12 lbs with clearly palpable ribs and good waist definition is healthier than a cat at 10 lbs where ribs are buried under fat. Use the BCS check to assess body condition rather than weight alone.
What does a BCS 6 or 7 cat look like?
+
BCS 6 (slightly overweight): Ribs are palpable but require more than light finger pressure to feel — there is a definite fat layer over them. From above, the waist curve behind the ribs is visible but less pronounced than ideal. From the side, the abdominal tuck may be absent or very slight. There may be a small fat pad at the belly, beyond the primordial pouch. At BCS 6, the cat is soft-looking but not yet obese — this is the critical stage to intervene before it progresses. BCS 7 (overweight): Ribs are difficult to feel even with firm pressure. No waist from above — the body is a tube shape. The belly is rounded or sagging. There may be obvious fat deposits over the hips/base of tail. At BCS 7, approximately 20–30% of body weight is fat. Health consequences: joint stress, diabetes (cats are especially prone to diabetes from obesity — feline diabetes mirrors type 2 human diabetes), fatty liver disease (hepatic lipidosis risk increases), increased anesthetic risk, and shortened lifespan. What to do: (1) Veterinary check to rule out hypothyroidism. (2) Measure ALL food accurately — most owners underestimate by 20–30%. (3) Reduce daily calories by 10–15%. (4) Switch to high-protein, low-carbohydrate food. (5) More play sessions — cats need interactive play, not free food. (6) No crash diets — cats who lose weight too fast develop hepatic lipidosis (a fatal liver disease).
Why is my cat fat even if it doesn't eat much?
+
Several causes beyond simple overeating: (1) SPAY/NEUTER EFFECT — the most common cause. Spaying or neutering reduces a cat's resting metabolic rate by 20–30% and increases appetite-driving hormones simultaneously. This is the #1 reason previously lean cats gain weight after 1–2 years post-surgery. Solution: reduce post-neuter food intake by ~25% and switch to a lower-calorie food. (2) INDOOR LIFESTYLE — indoor cats burn dramatically fewer calories than outdoor cats. Without hunting behavior (10–15 calories per "kill"), indoor cats are in constant calorie surplus unless food is actively managed. (3) FREE-CHOICE FEEDING — leaving food out all day ("free feeding") lets cats eat beyond hunger signals. Most cats on free-choice dry food gradually gain weight. (4) CALORIE-DENSE FOODS — dry kibble is very calorie-dense relative to its volume. Some cats feel full but have consumed far more calories than they need. (5) MEDICAL: hypothyroidism is rare in cats (unlike dogs), but Cushing's disease, insulinoma, or acromegaly can cause weight gain. If your cat is gaining weight despite eating less, bloodwork to check for endocrine disease is warranted. (6) AGE + MUSCLE LOSS — senior cats often lose muscle mass while gaining fat, so the scale barely changes but body composition worsens. BCS catches this; scale weight does not.
How do I help my cat lose weight safely?
+
CRITICAL RULE: Never fast a cat or reduce food drastically. Cats who stop eating for 2–3 days develop hepatic lipidosis (fatty liver disease) — a life-threatening condition. Weight loss must be slow and managed. SAFE APPROACH: (1) Calculate target caloric intake: typically 60–70% of what is needed to maintain IDEAL weight (not current weight). A vet or the tool below can help calculate this. For most overweight cats, 180–220 kcal/day. (2) Switch to a HIGH-PROTEIN, LOW-CARBOHYDRATE diet — wet/canned food is usually better than dry kibble for weight loss. High protein preserves muscle while losing fat; low carbs reduce insulin spikes that promote fat storage. (3) Feed 2–3 measured meals per day — NO free-choice feeding. Use a kitchen scale, not measuring cups (cups are inaccurate). (4) Eliminate treats OR use low-calorie treats: plain cooked chicken, a small piece of tuna, commercial low-calorie treats. No dry treats, which are often 5–10 kcal each. (5) Increase ACTIVE play — laser pointer, wand toy, feather toys for 15–20 minutes twice daily. This burns calories and satisfies hunting instincts that reduce stress eating. (6) Recheck BCS monthly. Target: 0.5–2% body weight loss per week maximum. A 5 kg cat should lose no more than 25–100 g/week. (7) If no progress after 6 weeks of strict diet: vet visit for bloodwork to rule out endocrine disease.
How often should I check my cat's body condition score?
+
Monthly BCS checks are ideal. Cats can silently gain 100–200 g per month — barely noticeable on the scale but adding up to 1–2 kg over a year. BCS catches this fat creep earlier than scale weight, because weight can appear stable even as fat replaces muscle (sarcopenia). HOW TO BUILD A HABIT: photograph your cat from the side and from above on the same day each month (e.g., the 1st of the month). Compare side by side. Also run the rib-feel test monthly — it takes 10 seconds. MORE FREQUENT checks recommended for: cats recently spayed/neutered (monthly for 6 months post-surgery, as this is when weight gain accelerates), cats on a weight loss program (every 2 weeks to monitor progress), senior cats (10+), cats with known endocrine disease. LESS FREQUENT OK for: lean young cats with stable lifestyle and diet (every 2–3 months). An important feline-specific note: if a previously food-motivated cat suddenly stops eating and loses weight rapidly, this is MORE urgent than gradual weight gain — rapid weight loss in cats triggers hepatic lipidosis risk even in obese cats. Any unplanned rapid weight loss in a cat = vet visit within 48–72 hours, not "wait and see."
More AI Pet Health Checks

Eye Infection Checker
Detect dog eye infection, cat eye problems, conjunctivitis, corneal ulcers, and cataracts.

Skin Disease Checker
Detect dog skin infection, cat skin problems, dermatitis, hot spots, and ringworm.

Dog Ear Infection Checker
Detect dog ear infection, ear mites, yeast infections, and ear discharge with AI photo analysis.

Cat Ear Mites Checker
Detect cat ear mites, ear infections, yeast infections, and ear discharge with AI photo analysis.

Cat Vomit Checker
Why is my cat vomiting? Analyze white foam, yellow bile, blood, hairballs, and more with AI.
Dog Vomit Checker
Dog vomiting when to worry? Analyze white foam, yellow bile, blood, and undigested food with AI.

Dog Nose Checker
Dog nose dry or runny? Analyze cracked noses, nasal discharge, and color changes with AI.

Dog Dental Checker
Detect dog tooth infections, gum disease, tartar buildup, and dental problems with AI photo analysis.

Dog Poop Checker
Blood in dog stool? Analyze poop color, detect worms, mucus, and diarrhea with AI photo analysis.

Cat Dental Checker
Detect cat tooth infections, gum disease, stomatitis, tooth resorption, and dental problems with AI photo analysis.

Dog Lump Checker
Found a lump on your dog? Identify skin tags, warts, cysts, lipomas, and bumps with AI photo analysis.

Cat Poop Checker
Blood in cat stool? Analyze poop color, detect worms, mucus, and diarrhea with AI photo analysis.

Dog Wound Checker
Is your dog's wound infected? Check infection signs, healing stages, and bite wounds with AI photo analysis.

Cat Lump Checker
Found a lump on your cat? Identify skin tags, cysts, lipomas, warts, and bumps with AI photo analysis.

Cat Nose Checker
Cat nose dry or runny? Analyze crusty noses, nasal discharge, and sneezing symptoms with AI.

Dog Paw Checker
Dog paw injured, swollen, or infected? Check cuts, yeast infections, peeling pads, and redness between toes with AI.

Dog Acne Checker
Pimples on your dog's chin or muzzle? Tell canine acne from mange with AI — includes puppy acne, severity stage, and treatment advice.

Dog Urine Checker
Blood in your dog's urine? Dark or orange pee? Check for UTI, dehydration, liver issues, or emergency signs with AI photo analysis.

Cat Paw Checker
Cat paw swollen, puffy, or injured? Check pillow foot, infections, abscesses, ingrown nails, and pad problems with AI.

Cat Acne Checker
Black specks on your cat's chin? Tell feline acne apart from flea dirt or mites with AI — includes severity stage and treatment advice.

Cat Urine Checker
Blood in your cat's pee? Dark or cloudy urine? Check color, clarity, and visible blood with AI — triage UTI, crystals, or liver issues.

Dog Gum & Tongue Checker
Pale, blue, yellow gums or black spots on tongue in your dog? Triage anemia, bloat, jaundice, toxin exposure, or benign lentigo with AI photo analysis.

Cat Gum & Tongue Checker
Pale, blue, yellow, or red gums/tongue in your cat? Triage FeLV, feline asthma, stomatitis, jaundice, or toxin exposure with AI photo analysis.

Dog Hair Loss Checker
Dog losing hair in patches, on tail, around eyes, or with no itching? AI identifies the pattern and ranks likely causes — ringworm, mange, flea allergy, or suspected endocrine disease.

Cat Hair Loss & Overgrooming Checker
Cat licking fur off, losing hair on belly, or scruffy coat? AI identifies miliary dermatitis, stud tail, ringworm, or flags paraneoplastic cancer warning in senior cats.

Dog Broken Nail Checker
Dog broken nail bleeding, hanging, exposed quick, or infected? AI assesses severity and gives step-by-step home treatment or clear vet-visit guidance.

Dog Body Condition Score Checker
Is your dog overweight, underweight, or ideal? Upload a side + top-down photo — AI scores body condition (BCS 1–9) and gives diet and exercise recommendations.

Dog Eye Discharge Checker
Green, yellow, clear, or brown eye discharge? AI identifies the color and ranks causes — bacterial infection, allergies, dry eye, porphyrin tear stains, or foreign body.

Cat Eye Infection & Discharge Checker
Green, yellow, brown, watery, or black crust eye discharge? AI identifies feline herpesvirus, chlamydia, URI, bacterial infection, or blocked tear duct — with urgency triage.
🐾
View All Tools
Explore all AI pet health check tools