Feline Stomatitis: Symptoms, Treatment, and Why Full-Mouth Extraction Works
Feline stomatitis (FCGS) causes severe, painful mouth inflammation in cats. Here's what it is, why cats cry yawning, and why many cats need full-mouth extraction for relief.
Published 2026-04-19

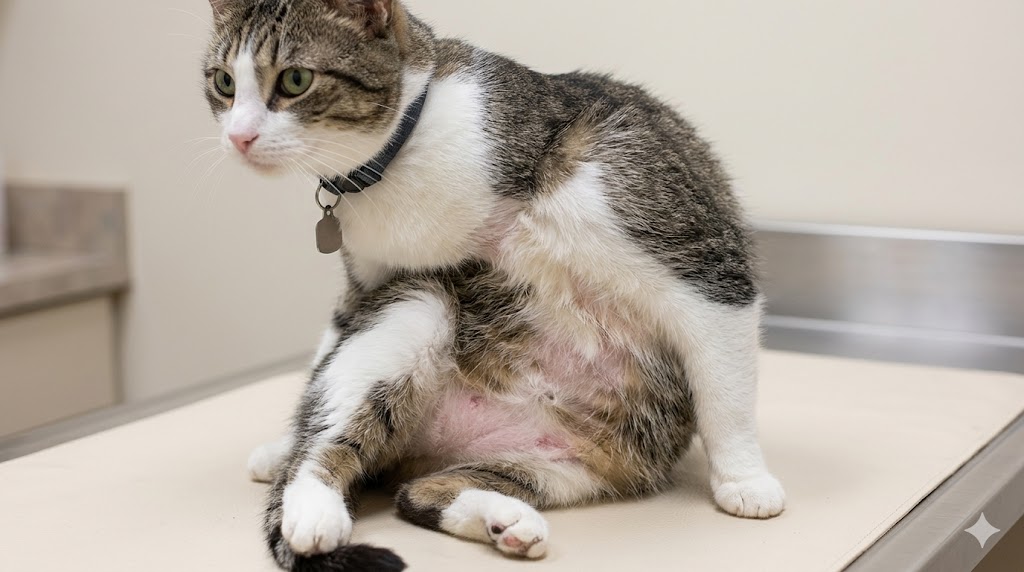
Feline chronic gingivostomatitis (FCGS), commonly called feline stomatitis, is one of the most painful oral diseases a cat can develop. Unlike typical gingivitis, stomatitis involves severe, widespread inflammation of the gums, inner cheeks, back of the throat, and sometimes the tongue — making basic activities like eating unbearably painful.
If your cat has been diagnosed or you suspect stomatitis, here's what you need to understand: the causes, symptoms, treatment options, and why full-mouth extraction — which sounds extreme — is actually the most effective long-term solution for most cats.
What Is Feline Stomatitis?
Stomatitis is NOT the same as normal gingivitis. Gingivitis is local inflammation right at the gum-tooth junction. Stomatitis is a severe, immune-mediated over-reaction — the cat's immune system massively overreacts to oral bacteria, causing inflammation far beyond what the level of dental disease would explain.
Think of it like an extreme allergy to the cat's own mouth bacteria. Even a small amount of plaque triggers a disproportionate immune response, leading to ulceration, swelling, bleeding, and severe pain.
Symptoms of Feline Stomatitis
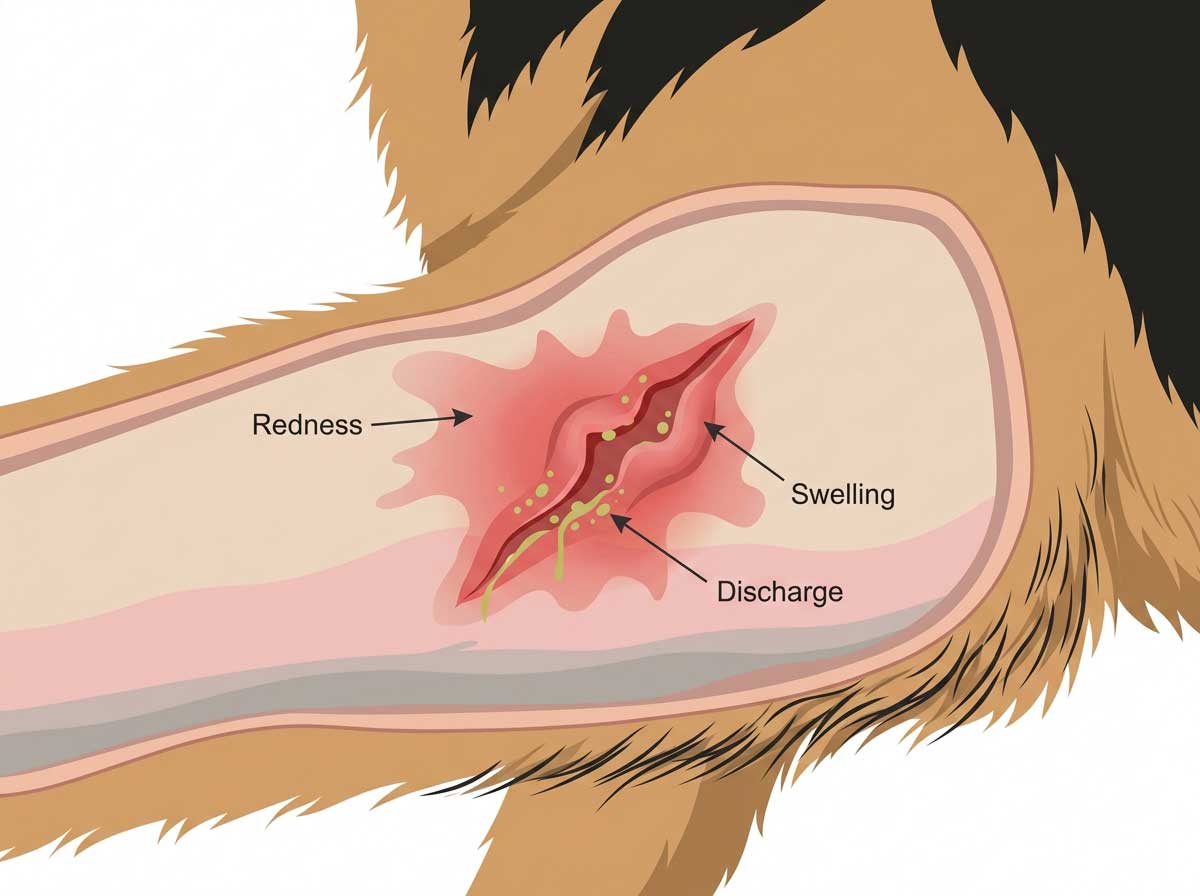
- ✓Bright red, swollen, inflamed gums extending well beyond the tooth line
- ✓Inflammation at the back of the mouth (caudal stomatitis) — often the most characteristic sign
- ✓Ulcers on the inner cheeks, gums, or tongue
- ✓Bleeding from the mouth during eating or spontaneously
- ✓Drooling — often excessive, sometimes blood-tinged
- ✓Crying or screaming when yawning (a hallmark sign)
- ✓Refusal to eat despite acting hungry — cat approaches food, tries to eat, then backs away
- ✓Preference for soft food and refusal of dry kibble
- ✓Weight loss due to reduced eating
- ✓Bad breath (halitosis) — severe and distinctive
- ✓Pawing at the mouth
- ✓Head shaking or squinting when chewing
- ✓Reduced grooming — painful to lick paws for cleaning
- ✓Hiding and avoiding interaction (pain-driven)
Causes — Why Do Cats Get Stomatitis?
The exact cause remains debated, but stomatitis is believed to be a combination of immune dysregulation and infectious triggers. Known associations and suspected causes include:
- ✓Feline calicivirus (FCV) — found in a majority of stomatitis cats
- ✓Feline Immunodeficiency Virus (FIV) — stomatitis often accompanies FIV
- ✓Feline Leukemia Virus (FeLV) — similar association with FeLV
- ✓Bartonella infection (cat scratch fever organism) — possible contributor
- ✓Genetic predisposition — some breeds seem at higher risk
- ✓Immune system dysregulation — the core mechanism; the cat's body reacts to normal mouth bacteria as if they were dangerous invaders
- ✓Concurrent dental disease that "primes" the immune reaction
Importantly: NOT every cat with FIV or FeLV develops stomatitis, and NOT every cat with stomatitis has FIV/FeLV. But testing for these viruses is standard when stomatitis is diagnosed because it changes management.
Do All Cats with Stomatitis Have FIV?
No — but FIV is a significant risk factor. Studies show roughly 15-30% of cats with stomatitis have FIV, compared to a baseline FIV infection rate of ~3-5% in the general cat population. The relationship works both ways: FIV can predispose cats to severe oral inflammation, and stomatitis should prompt FIV testing to rule it out. Any stomatitis diagnosis should include a SNAP combo test (FIV + FeLV) as part of the workup.
Treatment Options (In Order of Effectiveness)
1. Professional Dental Cleaning + Daily Home Care
For mild cases, a thorough dental cleaning under anesthesia followed by rigorous home care (daily brushing with a pet-specific toothpaste, chlorhexidine rinses) may control symptoms. Success rate: variable, works for maybe 10-20% of early cases. Most cats progress beyond this level of care.
2. Medications (Symptom Control)
Medications can reduce inflammation and pain but rarely cure stomatitis. Common options:
- ✓Prednisolone (oral steroid) — reduces inflammation; works but has long-term side effects and becomes less effective over time
- ✓Cyclosporine — immunosuppressant; helps some cats but requires monitoring
- ✓Antibiotics (clindamycin, amoxicillin-clavulanate) — control secondary bacterial infection; effect usually temporary
- ✓Pain medication (buprenorphine, gabapentin) — for comfort
- ✓Interferon-omega (Virbagen Omega) — immunomodulator; variable response
Medication-only management often costs $50-150/month indefinitely and many cats gradually lose response. It's a band-aid, not a cure.
3. Full-Mouth or Partial Extraction (Most Effective)
This is the game-changer. Removing all (or all back) teeth eliminates the plaque surfaces the immune system is reacting to. Without teeth, there's no plaque — and without plaque, the immune trigger is gone. Results:
- ✓60-80% of cats experience DRAMATIC improvement — from severe pain to essentially normal within weeks
- ✓15-25% experience partial improvement — still need some ongoing medication, but much less
- ✓5-10% have persistent refractory disease — extraction didn't solve it
- ✓Cost: $1,500-3,500 typical range depending on location, complexity, and imaging
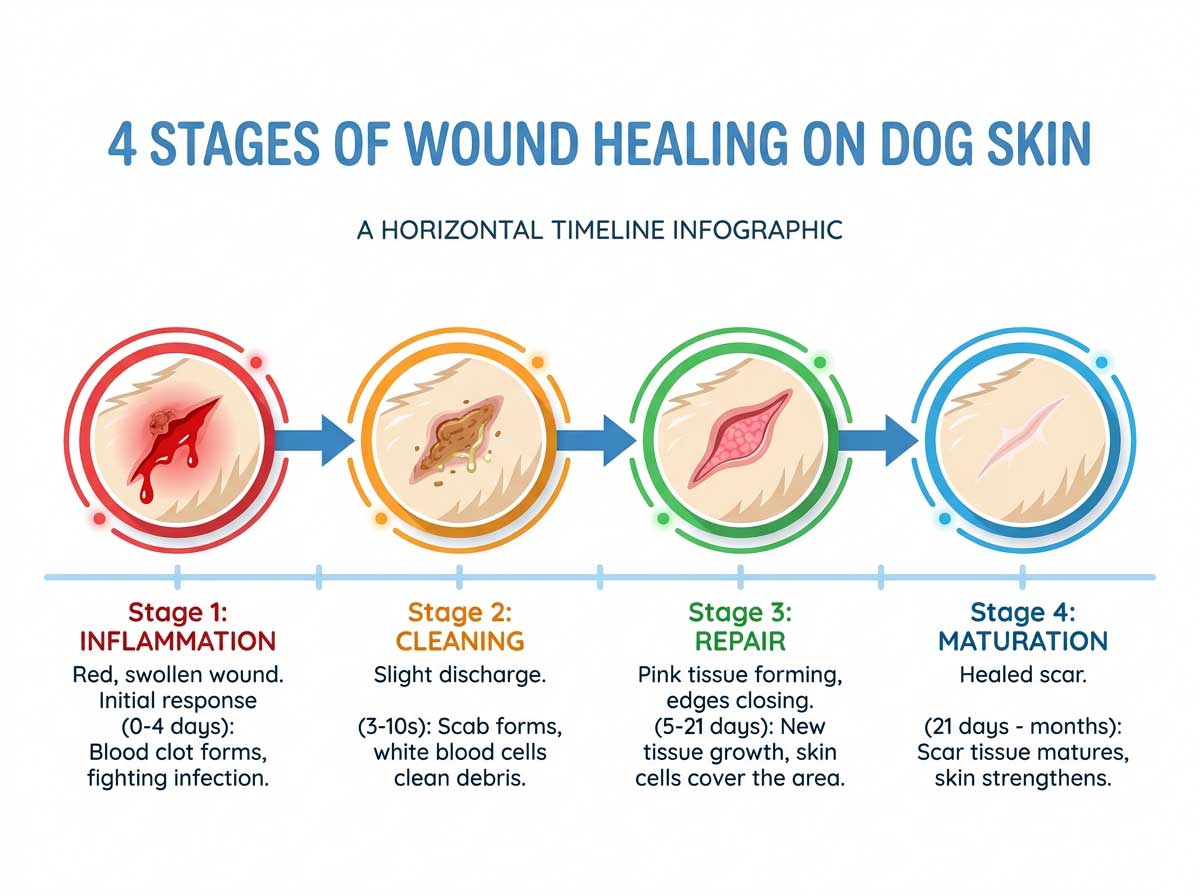
- ✓Recovery: 2-4 weeks for mouth healing; cats adapt to eating without teeth surprisingly quickly
Cats WITHOUT teeth can still eat dry kibble (they just gum it), wet food, or a mix. Many cats actually prefer the post-extraction state because the pain is finally gone.
How Long Do Cats with Stomatitis Live?
Stomatitis itself doesn't directly shorten a cat's lifespan. Treated properly (especially with extractions), most cats live normal lifespans. Factors that affect prognosis:
- ✓Response to extraction — cats with full response live essentially normal lives
- ✓Underlying FIV/FeLV — these can independently shorten lifespan
- ✓Weight maintenance — cats that eat well despite disease do best
- ✓Owner commitment — ongoing care matters
The real enemy with stomatitis is quality of life, not lifespan. Untreated stomatitis causes chronic severe pain — many cats stop eating adequately, lose weight, hide constantly, and have their lives dominated by oral pain. This is why aggressive treatment (including extraction) is recommended — it's about relieving chronic suffering, not just managing a condition.
New Treatments for Feline Stomatitis
Research is ongoing. Promising newer approaches include:
- ✓Mesenchymal stem cell therapy — an emerging treatment showing positive results in clinical trials for cats who don't respond to extraction
- ✓Laser therapy — CO2 laser for debridement and pain reduction
- ✓Toceranib phosphate (Palladia) — a tyrosine kinase inhibitor traditionally used for mast cell tumors, being trialed for refractory stomatitis
These are typically pursued for the 5-10% of cats who don't respond to extraction. For most cats, extraction remains the gold standard first-line curative treatment.
Is Feline Stomatitis Contagious?
Stomatitis itself is NOT directly contagious — the immune dysregulation doesn't transfer between cats. However, the viruses implicated (calicivirus, FIV, FeLV) ARE contagious between cats and can be carried from a cat with stomatitis to another cat. In multi-cat households with one stomatitis cat, have all cats tested for FIV/FeLV and vaccinated where appropriate.
When to See a Vet
If your cat shows any of these signs, schedule a vet appointment — the sooner stomatitis is diagnosed and treated, the better the outcome:
- ✓Refusing hard food or eating only soft food
- ✓Drooling or pawing at the mouth
- ✓Bad breath that's getting worse
- ✓Crying when yawning or eating
- ✓Weight loss
- ✓Bright red gums visible when lifting the lip
Not sure if your cat's mouth inflammation is stomatitis, gingivitis, or something else? Upload a photo of the mouth and gums — our AI can help identify stomatitis patterns vs normal gingivitis vs other oral conditions.
Stomatitis, Gingivitis, or Something Else?
Upload a photo of your cat's gums and mouth — AI identifies the inflammation pattern and severity in seconds.
Disclaimer: This article is for informational purposes only and is not a substitute for professional veterinary advice. Always consult a licensed veterinarian for diagnosis and treatment of your pet's health conditions.