Feline Tooth Resorption: The Painful Cat Disease Most Owners Miss
Feline tooth resorption (FORL) affects 30-70% of cats and causes severe pain — yet most owners don't know it exists. Symptoms, stages, treatment, and cost.
Published 2026-04-19

Feline tooth resorption (also called FORL — feline odontoclastic resorptive lesions) is one of the most common and most painful conditions in cats. 30-70% of cats over age 5 have at least one affected tooth. Yet many owners have never heard of it, because cats hide dental pain so well that the condition is usually silent until it's advanced.
Here's what every cat owner needs to know: what it is, how to spot it, why it hurts so much, and what treatment actually involves.
What Is Feline Tooth Resorption?
In tooth resorption, the cat's own body gradually destroys and absorbs the structure of its teeth. Specialized cells called odontoclasts attack the tooth enamel, dentin, and root — essentially dissolving the tooth from the inside or from the surface. Once the process exposes the pulp (nerve), the tooth becomes extremely painful.
This is NOT a cavity in the human sense — it's not caused by bacteria eating through enamel. It's an internal destructive process the cause of which remains unknown, despite extensive research. Theories include: immune-mediated, viral, dietary (excess Vitamin D), or a genetic predisposition — but none have been definitively proven.
Does Feline Tooth Resorption Affect All Teeth?
No, but it can affect multiple teeth. Patterns vary:
- ✓Some cats have just 1-2 affected teeth
- ✓Others have many teeth involved progressively over years
- ✓The most commonly affected teeth: premolars (especially the 3rd premolar) and molars in the lower jaw
- ✓Canine teeth and incisors are less commonly affected but not immune
- ✓Once a cat has one resorption lesion, the likelihood of developing more over time is high
This is why cats with one diagnosed lesion should have lifetime dental monitoring — new lesions appear over the years.
Symptoms — What You Might Notice
Cats are masters at hiding pain, especially dental pain. Even a cat with severe tooth resorption may appear to eat normally. Watch for subtle signs:
- ✓JAW CHATTERING when the affected area is touched (a classic sign — the cat's jaw will tremble or "chatter" involuntarily)
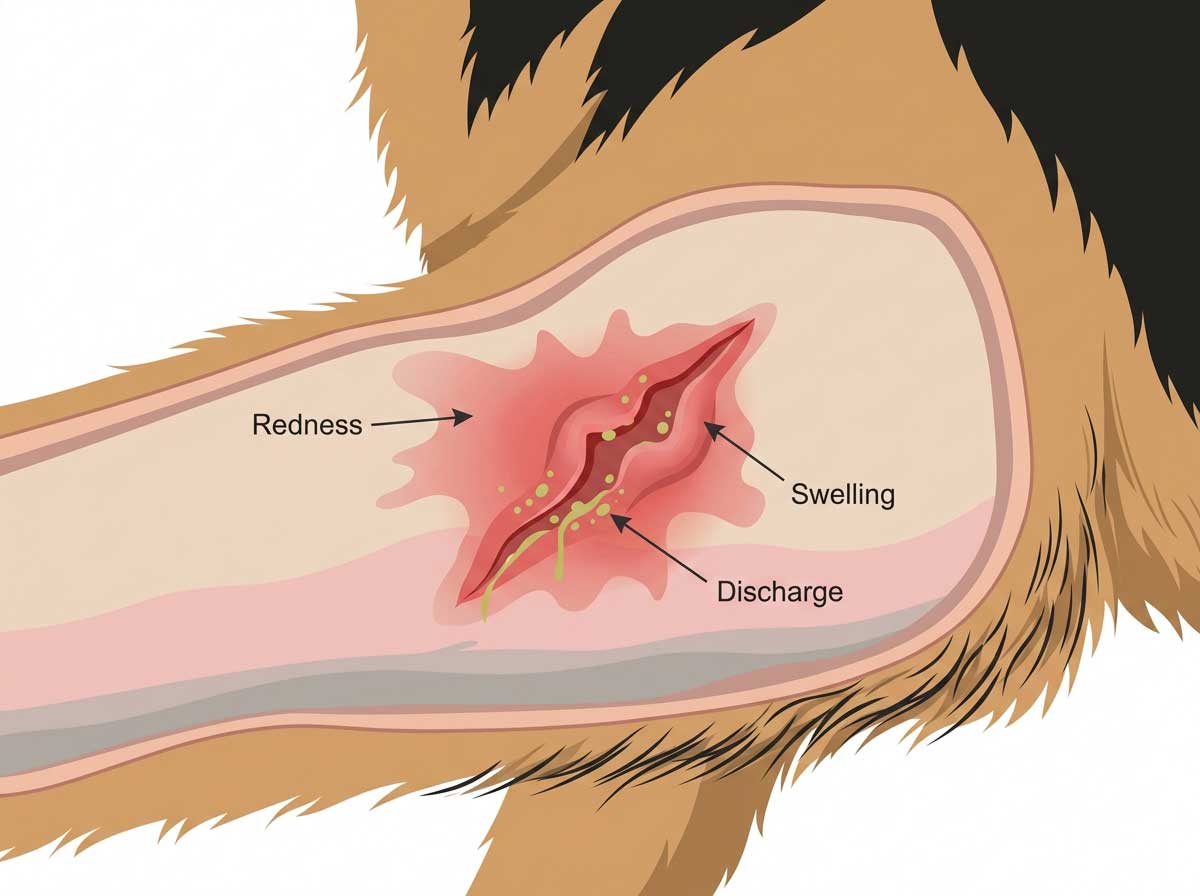
- ✓Bleeding from the gum at the tooth base — often you'll see a small red spot at the gumline where the lesion is
- ✓Red raised tissue growing up over the crown of the affected tooth (characteristic of resorption)
- ✓Dropping food while eating
- ✓Turning head sideways when chewing
- ✓Preference for soft food over hard
- ✓Drooling — sometimes only when eating, sometimes constant
- ✓Weight loss
- ✓Eating more slowly
- ✓Hiding or withdrawing
- ✓Reduced grooming — licking is painful
- ✓Halitosis (bad breath)
Most of these signs are subtle. Many cats are diagnosed during a routine vet exam when the vet touches the affected tooth and the cat jaw-chatters — a sign the owner may never have noticed at home.
How Painful Is Feline Tooth Resorption?
Extremely painful. When the lesion exposes the pulp (nerve), it's the equivalent of having severely exposed dental nerves constantly hit by food, saliva, and air. Cats endure this silently because instinct tells them hiding pain protects them from predators. Vets often remark that post-extraction, cats who had been slightly withdrawn or quiet for months "come back to life" — demonstrating how much chronic pain they had been hiding.
Stages of Feline Tooth Resorption
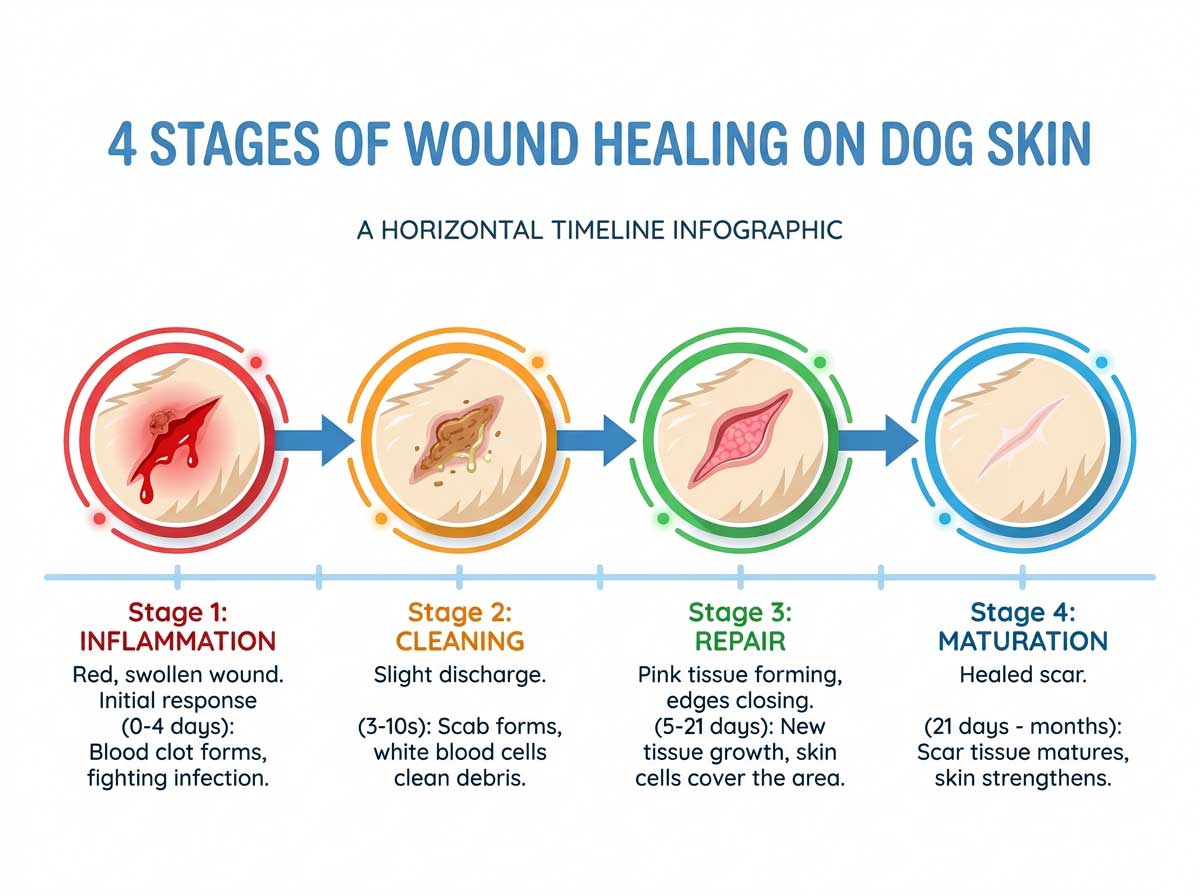
Veterinary dentistry recognizes 5 stages (based on extent of destruction visible on dental X-rays):
- ✓STAGE 1 — Mild hard tissue loss (cementum or cementum + enamel). Often not visible without radiographs. Usually not yet painful.
- ✓STAGE 2 — Moderate hard tissue loss, extending into dentin but not reaching pulp. Starting to cause pain.
- ✓STAGE 3 — Deep hard tissue loss extending into pulp. Very painful. Tooth needs extraction.
- ✓STAGE 4 — Extensive destruction; the tooth structure is severely compromised, sometimes just a crown over a destroyed root. Extraction essential.
- ✓STAGE 5 — Remnants of dental hard tissue only; the crown may be missing entirely, leaving only a gum-level scar. Usually no pain at this stage because the pulp is long gone.
Stages 3-4 are the most painful (active exposure of pulp). Stage 5 ironically is less painful because the destruction is complete. Diagnosis and staging require dental X-rays under anesthesia — external exam alone cannot stage the disease.
Treatment — What Actually Works
Unlike human cavities, resorption lesions CANNOT be filled. Fillings don't bond to resorbing tissue and the destructive process continues beneath any attempted restoration. The only effective treatment is extraction of affected teeth.
Extraction approaches:
- ✓SURGICAL EXTRACTION — the standard approach; the entire tooth (crown + roots) is removed. Requires a dental flap, bone removal, and suturing.
- ✓CROWN AMPUTATION (for specific Type 2 resorption cases) — the crown is removed but the roots are left to be fully resorbed by the body; acceptable only if the roots show NO periodontal ligament on X-rays. Requires specialist judgment.
Never allow crown amputation on a cat that hasn't had proper dental X-rays — leaving infected or still-vital root material causes ongoing pain.
How Much Does Feline Tooth Resorption Treatment Cost?
Typical costs in the US (varies by region, complexity, and whether a veterinary dental specialist is involved):
- ✓Dental examination + consultation: $50-150
- ✓Full-mouth dental X-rays (required for accurate diagnosis): $150-300
- ✓Anesthesia + dental cleaning: $300-600
- ✓Extraction of 1-2 teeth with resorption: additional $200-500
- ✓Multiple extractions (4+ teeth): $800-2,000+
- ✓Full procedure (exam + X-rays + cleaning + extractions): typically $1,200-3,500 total
- ✓Veterinary dental specialist: 1.5-2x general practice cost but worth it for complex cases
Pet insurance usually covers this if purchased before symptoms appear. Many cats need the procedure multiple times over their lifetime as new lesions develop — budget for periodic dental care.
What Happens If Tooth Resorption Is Untreated?
Untreated feline tooth resorption causes:
- ✓Chronic severe pain that the cat endures silently
- ✓Progressive weight loss and decreased quality of life
- ✓Secondary bacterial infection of exposed pulp, which can lead to tooth abscess
- ✓Spread of infection to surrounding bone (osteomyelitis of the jaw)
- ✓In rare cases, bacteria entering the bloodstream affecting heart valves or kidneys
- ✓Behavior changes — many cats become quiet, less interactive, or irritable
Tooth resorption doesn't kill cats directly, but it significantly impacts quality of life. Vets often describe post-extraction behavior change as "getting their cat back" — cats that seemed "just aging" turn out to have been in chronic pain.
Can You Prevent Feline Tooth Resorption?
Honestly — no, not reliably. Since the cause is unknown, there's no specific prevention. What you CAN do:
- ✓Regular home dental care — daily brushing (with cat-specific toothpaste, never human) reduces plaque that may contribute
- ✓Annual veterinary dental exams starting at age 3-5
- ✓Dental X-rays during annual cleanings to catch early-stage lesions before severe pain
- ✓Prompt treatment when lesions are found
- ✓Avoid giving cats hard chew objects (antlers, bones) that can break already-weakened teeth
How Do I Know If My Cat Has a Resorptive Lesion?
Early detection is hard without X-rays, but watch for:
- ✓A small red raised spot at the gumline of any tooth
- ✓Gum tissue growing up over a tooth crown
- ✓Jaw chattering when you touch the tooth area
- ✓Dropping food, chewing preferences, or mild dental-related behavior changes
- ✓Your cat is 5+ years old (prevalence rises with age)
If you notice any of these, schedule a dental exam. At the exam, ask specifically about tooth resorption — many owners don't know to ask, and some vets may not volunteer the diagnosis unless prompted.
Not sure if what you're seeing is tooth resorption, gingivitis, or stomatitis? Upload a photo of your cat's mouth — our AI can help distinguish the patterns.
Red Spot at a Tooth Base?
Upload a photo — AI can help spot the characteristic signs of tooth resorption vs gingivitis.
Disclaimer: This article is for informational purposes only and is not a substitute for professional veterinary advice. Always consult a licensed veterinarian for diagnosis and treatment of your pet's health conditions.